The National Institutes of Health has awarded the Oklahoma Medical Research Foundation $480,000 for Alzheimer’s research.
OMRF scientist Michael Beckstead, Ph.D., received a two-year grant to continue his study of the role the naturally occurring brain chemical dopamine may play in the earliest stages of Alzheimer’s disease.
Most current Alzheimer’s research focuses on the outer and upper sections of the brain, which control symptoms of the disease like memory loss. This study will instead focus on a small bundle of neurons near the base of the brain, which regulates dopamine function.
Dopamine is a chemical responsible for voluntary movement and the perception of reward in the brain. Beckstead studies what can happen when things go wrong with dopamine cells, ranging from Parkinson’s disease when too little is present to drug addiction when there is too much.
Scientists have not yet directly implicated dopamine in Alzheimer’s, but Beckstead said there is evidence to suggest it is involved in the initial stages of the disease.
“When you look at people who develop dementia, many of them were first diagnosed with depression or have a history of apathy,” said Beckstead, who holds OMRF’s Hille Family Foundation Chair in Neurodegenerative Disease Research. “These symptoms are closely linked to dopamine. There’s a good indication that the area handling the chemical could be involved years before tell-tale symptoms of Alzheimer’s appear.”
Scientists in Beckstead’s OMRF lab will observe dopamine-controlled behaviors in research models of Alzheimer’s throughout development and the impact of environmental changes like diet on disease progression.
The study will also include a partnership with OMRF scientist Bill Freeman, Ph.D., a researcher in the foundation’s Gene and Human Diseases Research Program. First, Beckstead’s lab will identify abnormal brain cells using electrical signals. Then, Freeman’s team will analyze the cells using a technique never before applied to Alzheimer’s disease models to look for clues to explain why they are behaving differently.
“We used to compare a region of an Alzheimer’s brain to a region of a normal brain,” said Freeman. “But we know within the brain there are many types of cells, and each could play a different role in Alzheimer’s. Now we can look at what’s different between individual dopamine neurons, which provides us with answers to better questions.”
Freeman said the partnership between labs is a natural result of the diverse talents at OMRF. “To do impactful science, you have to cross over multiple disciplines,” he said. “It’s always going to be a team effort.”
OMRF receives grant for Alzheimer’s research
Researcher, Educator, Leader Leaves Mark on Healthcare

During her long and distinguished career in nursing, Barbara Holtzclaw, Ph.D., R.N., has worked in three different but complementary worlds – providing care at the patient’s bedside; conducting research to improve that care; and educating the next generation to further the field through their own research.
It is the synergy of those three that has allowed her to advance the discipline of nursing in significant ways. Holtzclaw is retiring this summer as a research leader and professor in the Fran and Earl Ziegler College of Nursing at the University of Oklahoma Health Sciences Center, although as academicians are prone to do, it may be on paper only. She continues to conduct research and mentor nursing science students on the path she began many years ago.
“My research is a combination of my clinical experience, my curiosity of how physiological mechanisms work, and a mentor who showed me how nursing research can make a difference in clinical care,” she said. “Working with students allows me to foster their interest in nursing research the same way my mentor did many years ago.”
Holtzclaw is retiring as Associate Director of Translational Science for the Donald W. Reynolds Center of Geriatric Nursing Excellence at the OU College of Nursing. Prior to that, she served as Associate Dean for Research for the college, as well as interim director for the Ph.D. in Nursing program, which she helped to establish in 2008. Previously, she was a research director at the Vanderbilt University School of Nursing in Tennessee and Associate Dean for Research and Director of Doctoral Studies at the University of Texas Health Science Center in San Antonio. Joining the faculty at the OU College of Nursing in 2000 was like coming home – she earned her bachelor’s degree in nursing and a doctorate in higher education from OU, and she directed a Family Nurse Practitioner certificate program and taught in the undergraduate and master’s degree programs at OU from 1968 to 1987.
Holtzclaw was introduced to nursing research in the 1970s while pursuing her master’s degree at the University of California at San Francisco, where her mentor was studying shivering in people who were being therapeutically cooled. During surgery, patients’ temperatures fall and their metabolisms decrease while they’re asleep, and for some procedures, like open heart surgery, patients are intentionally made hypothermic.
“That’s all fine while they’re asleep, but when they start to wake up, they start shivering,” she said. “When they shiver, their temperature rises and their blood pressure rises – there’s a heavy metabolic cost to shivering.”
Holtzclaw’s interest in the body’s thermoregulation only grew from there. She experimented with wrapping patients’ arms and feet – where the most dominant sensors are – in three layers of terrycloth toweling to see if she could prevent shivering even though the patient was being cooled. During her post-doctoral fellowship at the University of Pennsylvania, her research delved further into post-operative temperature change and the negative effects of such energy expenditure. At an annual meeting of the American Society of Anesthesiologists, she presented the results of her study, conducted with a cardiovascular anesthesiologist, which established shivering as the cause of a significant increase in metabolic rate and cardiac effort.
“During the study, I remember pointing out to a new doctor that his patient was shivering, and he said, ‘Well, how do you expect them to get warm?’ I responded, ‘Would you have your patient go out and shovel snow?’ I went on, ‘No, but your patient is using the same amount of oxygen and is under as much metabolic stress as if they were shoveling snow.’”
Holtzclaw’s research expanded to investigate shivering in patients with cancer who were taking an antifungal drug called Amphotericin B. The body responds to the drug by running a fever and shivering, not because the patient is actually cold, but because the drug tricked their nervous system into raising its thermostat to a higher level, so it thinks they’re cold. The wrapping intervention worked to suppress shivering. She then studied the same phenomenon in patients with HIV who had opportunistic infections with high fevers, and again the wrapping intervention worked. All along the way, her research raised awareness among nurses and physicians about the risks of shivering.
“It has been satisfying to find a research area that affects almost every walk of life,” Holtzclaw said. “Shivering doesn’t happen by itself – it happens within all these other scenarios. That has allowed me to take my research in slightly different directions regarding thermoregulation.”
More recently, Holtzclaw has been working with a graduate student on the concept of immunosenescence – the gradual deterioration of the immune system with age – and its effect on vaccine response in older adults. These effects lower older adults’ protection against the virus, even with vaccination, which points to the extra precautions needed with this age group, she said.
During her career, Holtzclaw published two books, wrote numerous articles, and gave presentations around the world on the topics of fever, shivering and hypothermia. She was founding editor of the Southern Online Journal of Nursing Research and continues to serve on review panels and advisory boards for numerous other journals. She is a fellow of the American Academy of Nursing and the Gerontological Society of America, among many other honors.
While her research has been highly regarded, Holtzclaw has also played a significant, but sometimes behind-the-scenes, role as educator and mentor to many students.
“Dr. Holtzclaw has been absolutely committed to mentorship, which includes students, early-career colleagues, senior colleagues, and others outside the discipline. She always finds ways to help people be successful,” said Lazelle Benefield, Ph.D., R.N., Professor and Dean Emeritus of the OU College of Nursing and director of its Donald W. Reynolds Center of Geriatric Nursing Excellence.
OU College of Nursing Dean Julie Hoff, Ph.D., MPH, R.N., added, “Students, faculty and staff have all been touched by Dr. Holtzclaw’s passion for teaching, research and nursing.”
The OU College of Nursing is part of the OU Health Sciences Center, a leader in education, research and patient care and one of only four comprehensive academic health centers in the nation with seven professional colleges. To find out more, visit nursing.ouhsc.edu.
Photography Exhibition Exploring Nuclear History in New Mexico Opens at OU Art Museum


A new exhibition featuring acclaimed American photographer Patrick Nagatani’s (1945-2017) portfolio that addresses nuclear testing, waste and history in the state of New Mexico opens Thursday, Aug. 5, at the Fred Jones Jr. Museum of Art, located on the University of Oklahoma Norman campus. Nuclear Enchantment, a series of 40 images created by the artist between 1988 and 1993, plays upon New Mexico’s motto as the “Land of Enchantment” to raise awareness of the effects of the nuclear industry on the state’s land and people. This is the first time the entire series has been exhibited in Oklahoma.
After moving to New Mexico in 1987, Nagatani visited sites of nuclear testing and radiation in the state. He saw parallels between narratives constructed around the nuclear industry and those found in the Hollywood film industry, where he had previously worked as a set designer. “The story Nagatani reveals through vivid colors and outlandish compositions may surprise, even disturb, viewers about the region many of us escape to during hot Oklahoma summers,” said curator Hadley Jerman. “The fabricated scenes and distorted landscapes are fascinating accounts of the stranger-than-fiction tale of nuclear testing in New Mexico but also serve as pointed commentary on photography’s role in “recording” the past.”
This exhibition is made possible by the generous recent gift of the series to the museum from the FJJMA Association and the Andrew Smith Gallery. In a time when museum galleries across the nation, and the world, were shuttered for the better part of the past 18 months, the acquisition of this portfolio helps meet the museum’s mission of bringing diverse art for public display at the Fred Jones Jr. Museum of Art. “We are excited and grateful for this opportunity to expand the museum’s collection with this striking, imaginative series,” said Alison Fields, a faculty member at OU’s School of Visual Art and co-interim director of the museum. “The issues raised in Nuclear Enchantment remain relevant today, and we look forward to sharing Nagatani’s important work with the public.”
In Nuclear Enchantment, Nagatani makes visible a New Mexico whose “enchanting” vistas are poisoned by toxic waste and whose arsenal—whether celebrated in monuments or missile displays outside schools—continues to threaten New Mexico’s inhabitants, specifically Native Americans. Before his untimely death in 2017, Nagatani wrote, “My intentions are to raise public consciousness about the effects of New Mexico’s nuclear industry that continues to grow despite the damage it has already caused and will continue to bring to the state. The series, Nuclear Enchantment, attempts to awaken the many New Mexicans who still believe nuclear power poses no threat and that defense spending promotes the economy. Culturally and geographically connected to New Mexico, it is perceived by the elite powers as a place that can be abused and even reduced to rubble.”
Patrick Nagatani: Nuclear Enchantment, will be on display through January 30, 2022. Public programming for this exhibition will be announced at a later date.
GREG SCHWEM: I want my own Amazon spacecraft
by Greg Schwem
It never fails. All the good Father’s Day gift ideas appear after the holiday.
I don’t mean to sound ungrateful. I loved the barbecue tools and swimmer’s headphones that my wife and daughters gifted me last month. But had I paid more attention to Amazon founder Jeff Bezos’ space quest, my wish list might have looked very different.
Bezos, we all know by now, recently completed a short journey to space aboard something called the New Shepard rocket. Named for first man in space Alan Shepard and launched on the 52nd anniversary of the Apollo 11 moon landing, the craft returned safely and intact, allowing Bezos to resume duties as the world’s richest individual.
The capsule was completely automated, allowing Bezos and his three passengers to do absolutely nothing during the ride other than admire the views, the strongest evidence yet that space tourism could soon be a real thing.
As long as tourists are willing to climb into something that, no matter how you try and sugarcoat it, resembles the male phallus.
The design was confirmed by millions on social media who used it as additional fodder to unload on Bezos and his desire to spend billions on space travel while so many Americans live below the poverty line.
Seethe in anger all you want, Bezos haters. I will reserve judgement and applaud Bezos’ efforts, provided he agrees to run Blue Origin, his space exploration company, the same way he runs Amazon: Enable consumers to purchase whatever product their heart desires affordably and conveniently.
Admit it, isn’t that why we all use Amazon? We know that no matter what material good we see in a store, it can most likely be found cheaper on Amazon. We execute a few mouse clicks and then wait excitedly for whatever we ordered to arrive on our front porch. Well, we’re not always excited; the toilet brushes I recently ordered filled me with no adrenal rush whatsoever.
Bottom line? I want my own spacecraft, and I’m counting on Bezos to deliver it to me. I have ample room in my backyard to set up the launchpad. The area is also free of trees and power lines, ensuring a safe and unencumbered launch of my new spaceship.
Bezos’ three-person crew included a family member, his brother Mark. My only sibling lives eight hours away, but my wife enjoys quick getaways. Then again, she would probably prefer a little peace and quiet in the house, even if only for a quarter hour. So, I’ll leave her behind and ask a few of my male friends from the neighborhood. At least one needs to bring beer. Again, since computers will guide us through of our journey, there is no need to select a designated driver.
Once we return, we will have the ultimate excuse for laying on the couch and doing positively nothing. For as long as we desire. Demands that we get up and mow the lawn, take out the garbage or fold the laundry will be met with, “Hey, I was just in space!”
So, Jeff, please make good on my requests before late September, as my birthday falls at that time. Christmas at the latest. I have big plans for my spaceship in 2022.
Oh, and I’d also like free shipping.
(Greg Schwem is a corporate stand-up comedian and author of two books: “Text Me If You’re Breathing: Observations, Frustrations and Life Lessons From a Low-Tech Dad” and the recently released “The Road To Success Goes Through the Salad Bar: A Pile of BS From a Corporate Comedian,” available at Amazon.com. Visit Greg on the web at www.gregschwem.com.
You’ve enjoyed reading, and laughing at, Greg Schwem’s monthly humor columns in Senior Living News. But did you know Greg is also a nationally touring stand-up comedian? And he loves to make audiences laugh about the joys, and frustrations, of growing older. Watch the clip and, if you’d like Greg to perform at your senior center or senior event, contact him through his website at www.gregschwem.com)
Assisted Living Association to hold annual convention

Story by Bobby Anderson, RN
Oklahoma’s assisted living providers are set to gather later this month for the first time since Covid-19 in what Melissa Holland hopes to be a celebration and a learning event that will benefit Oklahomans.
The Oklahoma Assisted Living Association’s 2021 convention and trade show will be held Aug. 24-26 at RiverSpirit Casino Resort in Tulsa.
This year’s theme will be OKALA’s Roaring to Kick Off a New Decade with a 1920s flapper theme.
Melissa Holland, OKALA’s executive director, said this industry-only event will afford the opportunity for members to interact for the first time since Covid-19 in a comfortable, fun environment to share and learn best practices to serve the state’s assisted living population.
“We’re really excited because it will be an in-person event, back to our annual educational and trade show event,” Holland said. “We’ll have educational sessions for our administrators, nurses, activity directors, dietary, marketing and maintenance so they can come and get a lot of good education courses based on some of the needs they have expressed.”
Former University of Tulsa Head Football Coach and Oklahoma Senator Dave Rader will help kick off the event with a session on team building.
Holland said she frequently receives member requests on how to build strong, more cohesive staff units to better serve residents and Rader is one of the best in the field.
Having coached college football for four decades, Rader is best known for his 12 seasons as head coach of the University of Tulsa. At age 29 he was the youngest offensive coordinator in the Southeastern Conference. Then his alma mater made him the youngest head coach at the time in Division I NCAA football at the age of 31.
Awarded the NCAA District Coach of the Year honor in 1991 after his Freedom Bowl Champion University of Tulsa team finished 22nd in the national polls, he was appointed to the American Football Coaches Association Ethics Committee, and served as the representative of Independent Universities to the now defunct College Football Association.
Many of his student athletes went on to play in the NFL including seven quarterbacks, and many more to productive careers outside of athletics. His Tulsa teams consistently graduated at a higher rate than the university body in general.
He is honored to be a member of four Halls of Fame.
Walt Disney World/Epcot Center and Marriott Hotels alum Toni Fisk will present on her newly-released book #dinewithdignity Unlocking the Mystery of Dementia and Dining. Fisk brings her 35 years in the food and hospitality to bear in tackling an often overlooked senior issue.
The book focuses on the role of care partners and provides insight and tips on ways to maximize enjoyment in the dining environment while answering “the questions that you didn’t know to ask.”
Holland said information will be presented on the Covid-19 vaccine and separating fact from fiction in today’s fragmented media environment.
The pandemic stretched providers in a number of directions in their efforts to keep residents and staff safe.
Holland said her members continued to rise to the occasion.
“They have been phenomenal. They really have,” Holland said. “They have been amazing. When they were locked down I was able to send them ideas and (information) to help them. I”ve never had so many thank-you’s in this last year-and-a-half.”
Assisted Living was founded on a resident-centered philosophy to enable choice, preserve dignity, encourage independence, and promote quality of life.
Assisted living communities offer supportive amenities, service and care in a residential setting with the comforts of home. Assisted living communities have a staff available 24/7 to assist with care, safety and support. When you have seen one assisted living community, you have just seen one. They come in all different shapes and sizes, and offer a variety of features, amenities and prices.
The association offers a number of resources to help you make an informed decision when evaluating the state’s 170 assisted living communities. You can visit their website at okala.org or call them at 405-235-5000.
ANA Supports Mandated COVID-19 Vaccinations
The American Nurses Association (ANA), representing the interests of the nation’s 4.2 million registered nurses, supports health care employers mandating nurses and all health care personnel to get vaccinated against COVID-19 in alignment with current recommendations for immunization by public health officials.
Increasing circulation of new variants, lagging COVID-19 vaccination rates, and continued public skepticism calls for nurses to uphold their professional and ethical obligations to model the same prevention measures as their patients. For our nation to maintain the momentum of recovery efforts from this persistent pandemic, enough individuals and communities must get vaccinated to reduce the risk of further infections, hospitalizations, and deaths.
“The scientific rigor to swiftly develop effective COVID-19 vaccines and the monumental efforts to ensure all Americans get vaccinated is nothing short of amazing. Vaccination is both a significant public health victory and a scientifically proven strategy to slow the spread of COVID-19 and prevent the loss of more American lives,” said ANA President Ernest J. Grant, PhD, RN, FAAN. “As the largest group of health care professionals, nurses are critical to all facets of COVID-19 response efforts and must strive to remain physically and psychologically safe to function optimally to care for themselves, their patients and their communities. Nurses must get vaccinated.”
ANA’s decision to support COVID-19 vaccine mandates for nurses aligns with its longstanding position on immunizations, which emphasizes that effective protection of the public health mandates that all individuals receive immunizations against vaccine-preventable diseases. ANA also believes that the safety profile of authorized COVID-19 vaccines is stable and has included the three COVID-19 vaccines being administered under the Food and Drug Administration’s Emergency Use Authorization. ANA maintains its stance to not support philosophical or religious exemptions as reasons not to get vaccinated.
“A significant number of nurses working in a variety of health care settings across the nation have diligently fulfilled their ethical duty to protect themselves, their colleagues, patients and loved ones by getting a COVID-19 vaccine,” said Dr. Grant. “We would absolutely be remiss to not acknowledge these nurses and applaud them for leading the charge and setting an example for their patients.”
In a survey of over 22,000 nurses conducted by the American Nurses Foundation between January 19 and February 16, 70% of nurses said they had received at least one COVID-19 vaccine. Most recently, in a survey of over 4,500 nurses conducted by the COVID-19 Facts For Nurses Campaign between April 12 and May 4, 83% of nurses reported that they had received the recommended dose regimen of two COVID-19 vaccine shots.
Nurses might desire more understanding about the safety profile of COVID-19 vaccines as they decide whether to get vaccinated and there are legitimate reasons that a nurse might decide not to take the COVID-19 vaccine, such as severe allergies, compromised immune systems, and other serious health conditions. ANA will continue to provide all nurses education and resources to guide their understanding and consideration of COVID-19 vaccines.
SAVVY SENIOR: Does Medicare Cover Home Health Care?
Dear Savvy Senior, How does Medicare cover in-home health care? My husband has a chronic health condition that makes it very difficult for him to leave the house, so I’m wondering if he could qualify for Medicare home health care.
Seeking Help
Dear Seeking,
Medicare covers a wide variety of part-time or intermittent in-home health care services to beneficiaries in need, if they meet Medicare’s criteria. Here’s how it works.
In order for your husband to secure coverage for home health care, Medicare first requires that he be homebound. This means that it must be extremely difficult for him to leave home, and he needs help doing so either from another person or medical device like a cane, wheelchair, walker or crutches.
He will then need to have a face-to-face meeting with his doctor to get a home health certification confirming that he needs skilled-nursing care or skilled-therapy services from a physical or speech therapist on a part-time basis.
His doctor can also request the services of an occupational therapist and a personal care aide to assist with activities of daily living such as bathing, dressing and using the bathroom. His doctor must renew and certify his home health plan every 60 days.
He will also need to use a home health agency that is certified by Medicare.
If he meets all of the requirements, Medicare should pay for his in-home health care.
But be aware that Medicare will not pay for personal care aide services (for bathing, dressing, using the bathroom, etc.) alone if he does not need skilled-nursing or skilled-therapy services too. Homemaker services, such as shopping, meal preparation and cleaning are not covered either.
If your husband has original Medicare, you can locate a Medicare-certified home health agency by calling 800-633-4227 or by visiting Medicare.gov/care-compare. If he has a Medicare Advantage plan, you should contact his plan directly and ask which home health agencies work with the plan and are within the plan’s network of providers.
For more detailed information on how Medicare covers in-home health, see the “Medicare and Home Health Care” online booklet at
Medicare.gov/Pubs/pdf/10969-Medicare-and-Home-Health-Care.pdf.
Other Options: If your husband does not qualify for Medicare home health care coverage, there are other coverage options depending on your situation. Here are several that may apply to you:
Insurance: If you happen to have long-term care insurance, check to see if it covers in-home care. Or if you have a life insurance policy, see if it can be utilized to pay for care.
Medicaid: If your income is low, your husband may qualify for Medicaid, which offers different home and community-based services that can pay for in-home care. To investigate this, contact your local Medicaid office.
Also see if PACE – which stands for “Programs of All-Inclusive Care for the Elderly” – is available in your area (see NPAonline.org). PACE provides in-home care, including help with activities of daily living, such as meals, dental and medical care, among other benefits.
Veterans Benefits: If your husband is a veteran, the VA also offers some benefits that can help. Two programs to inquire about are “Aid and Attendance or Housebound Allowances” and the “Veteran-Directed Care” program. Both programs provide monthly financial benefits to eligible veterans that can help pay for in-home care. To learn more, contact your regional VA benefit office (see Benefits.va.gov/benefits/offices.asp or call 800–827–1000).
To look for these and other programs in your area that can help pay your husband’s home care, go to PayingForSeniorCare.com and click on “Find Financial Assistance for Care” to access their Eldercare Financial
Send your senior questions to: Savvy Senior, P.O. Box 5443, Norman, OK 73070, or visit SavvySenior.org. Jim Miller is a contributor to the NBC Today show and author of “The Savvy Senior” book.
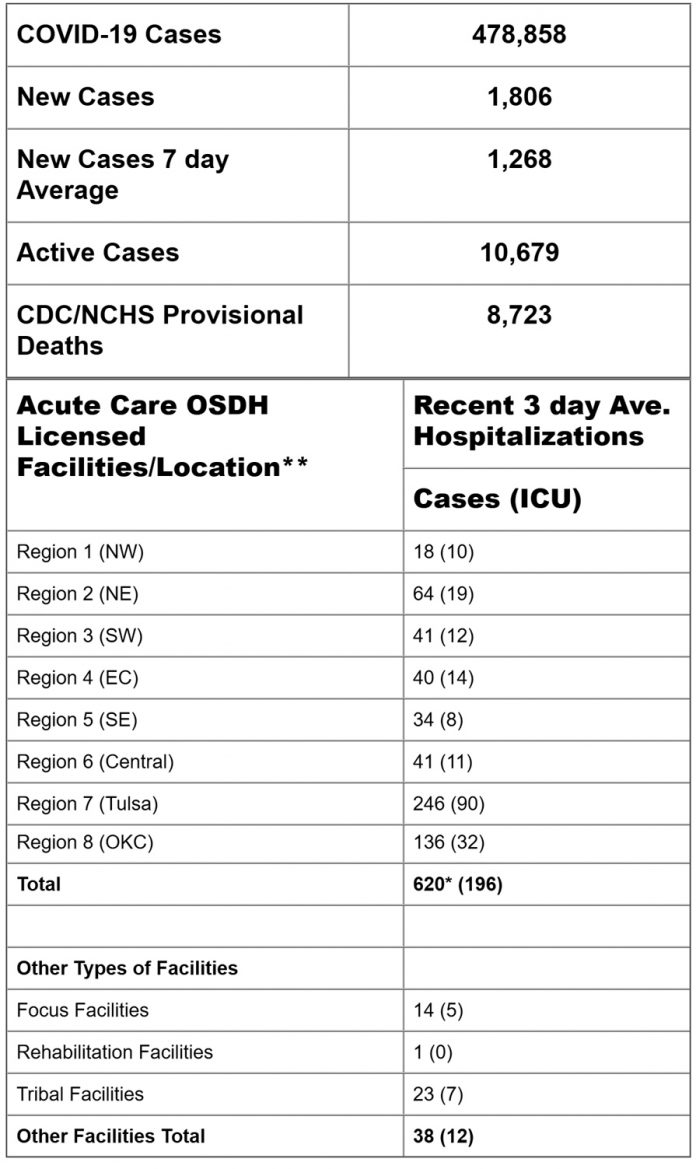
SITUATION UPDATE: COVID-19: COVID-19 Oklahoma Test Results
* *Includes 27 pediatric hospitalizations.
**Focus, Rehabilitation and Tribal Facilities numbers are not assigned to a specific region as their patient populations reside across the state. Information provided through survey of Oklahoma hospitals as reported to HHS as of the time of this report. Response rate affects data. Facilities may update previously reported information as necessary.
Data Source: Acute Disease Service, Oklahoma State Department of Health. *As of 2021-07-29 at 7:00 a.m.
OK Living Choice Program assists Seniors transition out of nursing home
Do you have a loved one in a nursing facility that needs assistance transitioning back into the community? Oklahoma Living Choice Program may be what you are looking for. The Oklahoma Living Choice Program assists Oklahomans wanting to transition out of a nursing home and back into the community in a residence of their own. The populations served are individuals 65 and over, and individuals 19 and up with a physical disability.
To qualify for the Oklahoma Living Choice Program one should meet the following:
* Be at least 19 years of age
* Qualify for SoonerCare (Oklahoma’s Medicaid Program) for at least one day prior to transition
* Have lived in an institutional setting (nursing home) for at least 60 consecutive days
* Voluntarily want to transition back into the community
* Be willing to play an active role in his/her plan of care
Depending on the individual’s needs there are many services that the Oklahoma Living Choice Program offers, such as: assistance finding a new home, home delivered meals, transportation, skilled nursing, therapy services, personal care, medication management, and there are transitional funds (a one-time allotment of up to $2,400).
Anyone can refer a potential individual that resides in a nursing home for the Oklahoma Living Choice Program by accessing the online referral form http://www.okhca.org/ReferralHome.aspx?ref=LC
If you need more information or have questions about the Oklahoma Living Choice Program you can contact 888-287-2443 or email [email protected]
If you have a loved one in a Long-Term Care facility and have any questions regarding any concerns you may have, you can contact an ombudsman to assist you.
Areawide Aging Agency Long-Term Care Ombudsman Program advocates for the needs of residents in LTC facilities serving Canadian, Cleveland, Logan, and Oklahoma Counties. You may contact us at (405)942-8500.
The Cowboy Seeks the Best Volunteers in the West
The Cowboy invites individuals with a passion for the history and stories of the American West to join the team of volunteers and docents that help keep the Museum running.
“We have an amazing team of volunteers at the Museum who are committed to life-long learning and sharing the American West with our visitors,” said Natalie Shirley, National Cowboy & Western Heritage Museum President and CEO. “One of the most amazing things about the Cowboy is how committed our volunteers are to creating an environment where anyone can come and learn.”
Volunteer docents serve as guides in the galleries, frequently leading tour groups and working closely with children through educational programs. “Volunteering is an excellent way to make a difference in other people’s lives, as well as your own life,” said Todd Bridgewater, Manager of Volunteer Engagement at the Museum. “People come from all walks of life and find a home here, whether they are a cowboy or not.”
Those interested in becoming a docent can complete a Volunteer Application online by visiting nationalcowboymuseum.org. New docent orientation is Tuesday, August 17, 2021, from 9:00 a.m. – 12:00 p.m. Training begins Thursday, August 19 and occurs every Tuesday and Thursday through September 23, 2021. Training times vary but are generally between 8:30 a.m. – 4:30 p.m. For a detailed description of the docent role and its commitments, CALL (405) 478-2250.
Nationally accredited by the American Alliance of Museums (AAM), the National Cowboy & Western Heritage Museum is located only six miles northeast of downtown Oklahoma City in the Adventure District at the junction of Interstates 44 and 35, the state’s exciting Adventure Road corridor. The Museum offers annual memberships beginning at just $40. For more information, visit nationalcowboymuseum.org. For high-resolution images related to the National Cowboy Museum, visit nationalcowboymuseum.org/media-pics.